While dealing with medical equipment in laboratories or hospitals, the chances of cross-contamination are significantly higher. This contamination can be the reason behind the transfer of infection to the patient which, in some cases, can have disastrous outcomes. Therefore, it is necessary to, not only sterilize every medical equipment before use but also to be sure of the quality of the sterilization process.
In this regard, the role of indicators is prominent. These are the means through which the integrity of the sterilization process can be evaluated. These indicators are, although, of various types i.e. chemical and physical, the most reliable ones are the biological indicators.
What are biological indicators?
Biological indicators, abbreviated as BIs, are also called living indicators because, in this process, living organisms are employed as the indicating agent due to their higher sensitivity to the change in environmental conditions.
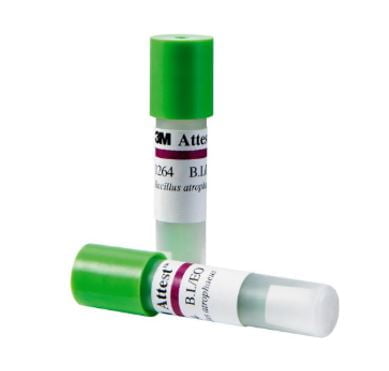
Biological indicators
These indicators include highly resistant bacterial spores. These spores are available in the form of ‘spore strips’ which are manufactured by sticking the bacterial spores onto a paper base. One such strip contains nearly one million bacterial spores. These are packed in a glassine envelope or a vial and are only opened prior to use.

Spore strips
Composition of the spore strips
The spore test uses highly resistant bacterial spores taken from different types of bacterial species to indicate the level of sterilization. The names of the types of bacteria used in this process are enlisted below:
- Geobacillus stearothermophilus: A soil-dwelling thermophilic bacteria which are capable of oxidizing carbon monoxide aerobically.

Bacterial endospores
- Bacillus atrophaeus: A black-pigmented strain of bacteria used in the field of biomedicine.
- Bacillus subtilis: A soil-dwelling bacteria which is also accustomed to dwelling in the mammalian intestinal tract. It is also called hay bacillus or grass bacillus.
How does a biological indicator work?
The following steps must be taken to conduct the spore test:
- Biological indicators are placed in a fully loaded sterilizer in which the sterilization is to be done.
- Once the process is started, the load as well as the biological indicator are subjected to sterilization.
- At the end of the process, the biological indicator is assembled into a mixture with incubation media and is also incorporated into a glass vial or ampule.
- This mixture is then incubated at the pre-specified temperature by the manufacturer.
- After the specified time period, the strips are taken out and the results are interpreted.
Interpretation of the results
With the use of spore strips, it is uncomplicated to read and interpret the results of the process which can be:
- Negative BI: If, after the incubation, the incubation media does not change color, it is an indication that the spores have been killed during the process. This ensures that the sterilization process is up to the mark in its efficiency.
- Positive BI: If the color does change, it is manifested that the sterilization process requires further adjustments as it is imperfect at the moment. In this case, further calibration of the sterilization process is required. Immediate steps must also be taken to quarantine the sterilizer and service it until a negative BI is obtained.
Types of biological indicators
The biological indicators, based on the time they require to produce the results, are classified into two categories:
- Standard biological indicators: In standard biological indicators, it is necessary to incubate the indicator after the test has been done in order to obtain the results. This process thus requires more time, i.e. two to three days, to indicate whether the sterilization process is efficacious or not.
- Rapid readout indicators: In the case of rapid readout indicators, a certain type of reactive enzymes are used to produce quick results i.e. within one to three hours.

Rapid readout biological indicator test
Where the biological indicators are employed?
The biological indicators can be applied to check the efficacy of the following processes:
- Steam sterilization
- Ethylene oxide sterilization
- Dry heat sterilization
- Autoclaving process
- Clean rooms
- Biological safety cabinets
- Isolators
Advantages of the biological indicators
The biological indicators provide the following advantages:
- The biological indicators ensure the lethality of the process of sterilization.
- Biological indicators generate relatively more accurate results in comparison to those obtained by chemical or physical indicators.
- These indicators, by working correctly, reduce the chances of the transmission of infections to the patient thus reducing the health burden on the health department.
Demerits of using biological indicators
Although biological indicators are the most reliable way of measuring the efficiency of the process of sterilization, here are some of the demerits associated with their use:
- The biological indicators are to be used on a weekly basis as they require 24 to 48 hours of incubation before giving the results. Because of this, their daily use is a complicated process.
- A significant time duration is required to obtain the results with the standard biological indicators. This issue can be resolved by the use of rapid readout indicators which are at power with the standard biological indicators in terms of efficiency.
Conclusion
Sterilization is one of the most important processes being used in hospitals as well as industries on a daily basis. It ensures that no bacteria passes to the patient through the employment of a medical apparatus. But this sterilization equipment also requires regular calibration which makes sure that they are working properly. Here, the employment of indicators comes into the process. Among the other available options, biological indicators are preferred over the others due to their accuracy of the results. They are available in the form of spore strips which are easy to use during the process as well as easy to read and interpret afterward. Hence, biological indicators are widely used substances in hospitals and industrial setups.

PhD Scholar (Pharmaceutics), MPhil (Pharmaceutics), Pharm D, B. Sc.
Uzma Zafar is a dedicated and highly motivated pharmaceutical professional currently pursuing her PhD in Pharmaceutics at the Punjab University College of Pharmacy, University of the Punjab. With a comprehensive academic and research background, Uzma has consistently excelled in her studies, securing first division throughout her educational journey.
Uzma’s passion for the pharmaceutical field is evident from her active engagement during her Doctor of Pharmacy (Pharm.D) program, where she not only mastered industrial techniques and clinical case studies but also delved into marketing strategies and management skills.
Throughout her career, Uzma has actively contributed to the pharmaceutical sciences, with specific research on suspension formulation and Hepatitis C risk factors and side effects. Additionally, Uzma has lent her expertise to review and fact-check articles for the Health Supply 770 blog, ensuring the accuracy and reliability of the information presented.
As she continues her PhD, expected to complete in 2025, Uzma is eager to contribute further to the field by combining her deep knowledge of pharmaceutics with real-world applications to meet global professional standards and challenges.